Nikki Harris
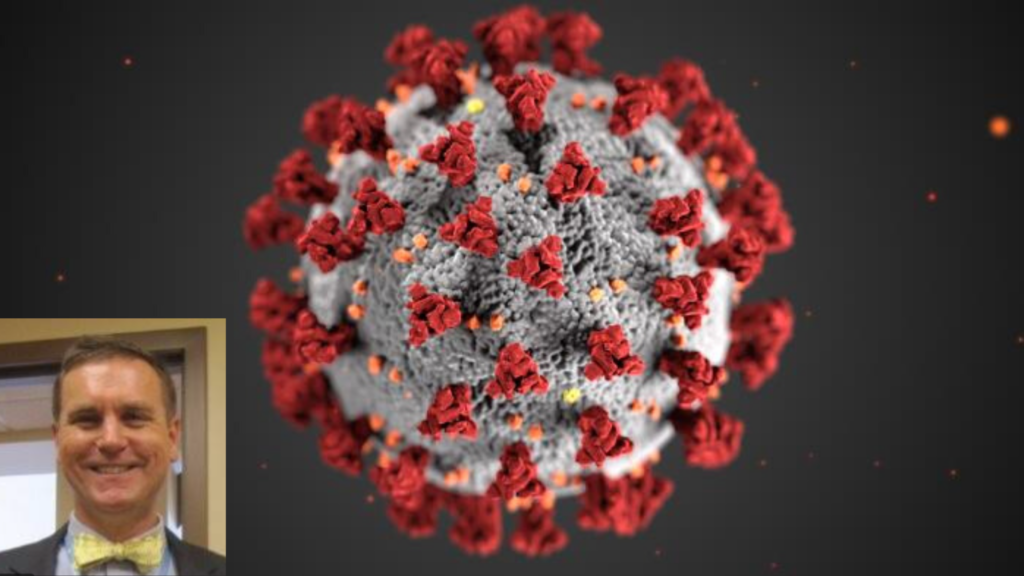
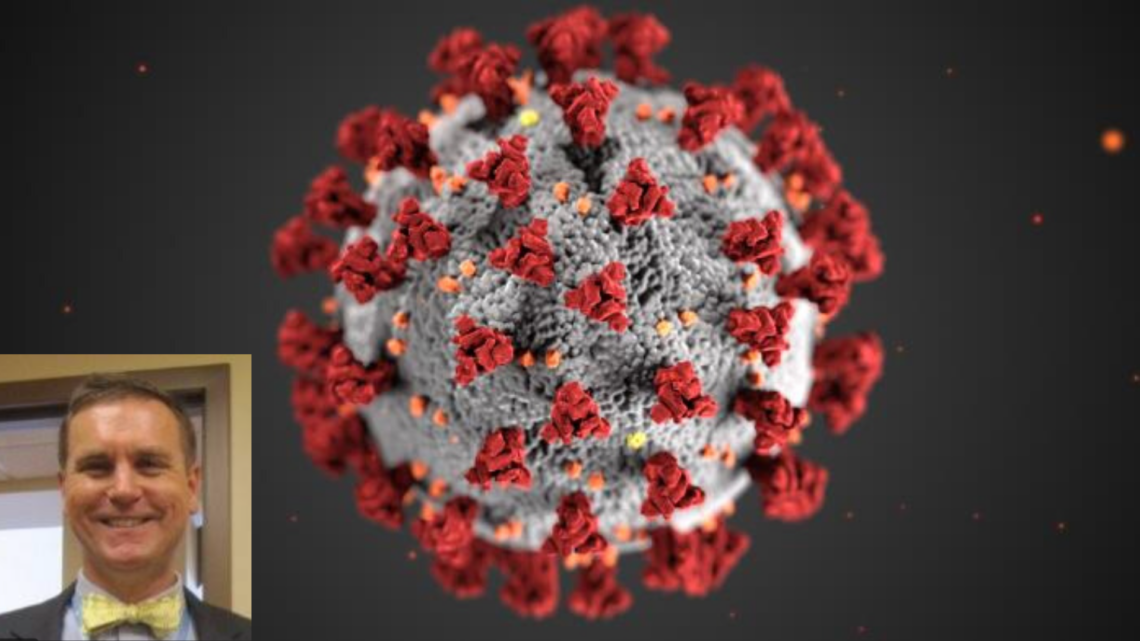
The following is the transcript of an interview with Dr. Stephen Haering, director of the Alexandria Health Department, on the state, local and federal response to COVID-19; the availability of tests and medical equipment; and the reopening of Virginia. When the interview was conducted on April 19, there were 300 confirmed cases of COVID-19 in Alexandria. As of April 20, Alexandria has over 400 cases, including 8 fatalities.
This interview has been edited and condensed for brevity and clarity.
Harris: What does a normal weekday look like for you these days? What’s your role in mitigating this pandemic?

Haering: There is no normal weekday. As the health director, I oversee the environmental health, the clinical public health specialty clinics, the population health team, and the administrative division of the Health Department. A lot of it is supporting my staff, who are doing the work on the frontlines, and that can be anything from really helping them to solve the problems that they are encountering, and interacting with our community partners, both the city agencies, as well as the nonprofit and other organizations, both in the city of Alexandria and regional. We in the city have a meeting every day to discuss what is going on and strategize for the next week.
Harris: Can you give a rough estimation of where we are right now on the curve and when we will reach the peak?
Haering: You know, we are not able to make that assessment. Modeling is actually a very complex undertaking. The primary reason is that this is a brand new virus to the human species, so we and public health officials are still categorizing much of the characteristics of this. How long is the presymptomatic period that one is infectious? How many people are asymptomatic with the infection? We have some pretty good statistics or ideas in terms of the number of people who get sick and need hospitalization and intensive care. But, in terms of being able to model where the peak is going to be, we are really focused on looking at how we will know that we can make modifications to the shutdown, the stay-at-home orders. And one of the key parts of that is going to be increased testing. It is very difficult to reopen successfully if we do not have widespread testing.
Harris: What are the criteria for getting a test right now in Alexandria?
Haering: It depends on how you’re looking at it. The criteria for actually doing the testing are set by each individual clinician’s office who’s doing the test. Most of them are following the Centers for Disease Control and Prevention (CDC) recommendations for prioritizing. And one of the criteria, of course, is to actually have an illness, a fever, a cough, shortness of breath, to have the sort of symptoms that the coronavirus has. If we back up, in the progress or the history of what has happened, is that when the virus was first detected, the only lab in the country that was doing the testing was the CDC. Within a couple of weeks of that time, after the CDC had their labs set up, then state public health labs started to do it. It is a complicated process to do a lab test and get it accurate. And, so, when the state public health labs were the only labs doing it, in addition to the CDC, the criteria were very narrow.
Now that there are private labs doing it, like Lab Four, those private labs do not have any criteria. And so it’s really up to the individual health care systems–the hospitals and the private practices to decide who they are testing. In the state public health lab, there is no collection of the tests, so the collection is determined by the healthcare provider. LabCorp and Quest Diagnostics will run it for anybody they receive a test for. State public health labs are being used for people who are in congregate living facilities — group homes, assisted living homes, or long-term care facilities — and for critical infrastructure, in other words, first responders–firefighters, police, and health care workers.
Harris: Do you have any expectations on when tests will be widely available?
Haering: That’s a question we all have in public health, the community, in the media. Because that is part of the healthcare system that drives that, I don’t really know when that will happen. I know even New York and New Jersey, who are in the throes of a really profound epidemic, are calling for more tests. We all are calling for more tests. And because there is no overarching, unified, healthcare system–it’s more of a healthcare sector–that is driven by the market forces. And, quite frankly, just like the personal protective equipment (PPE), it’s not being organized nationally.
Harris: So all the PPE, ventilators, and testing are coming from the private sector?
Haering: That is correct. The public Health Department doesn’t do anything about ventilators, but the hospital systems are getting that stuff through the private sector. There’s a number of different groups that are using the PPE. Of course, the health care workers are, but also the health care workers in group homes and long-term care facilities, and they get theirs through the private sector. The Health Department has had access to PPE through the Strategic National Stockpile (SNS). And we have distributed the PPE that we have received from the SNS to healthcare providers who are doing testing as well as long-term care facilities. The PPE involves goggles, masks, gowns and gloves.
Harris: Is Alexandria competing for PPE or is that the state’s role to distribute what they receive from the SNS?
Haering: It is allocated based on the size of the population. There is a number of different sources for the PPE. One is the SNS. And another is through the Northern Virginia Health Care Association, which supports long-term care facilities. That is a separate entity from public health. And the main source is through the private sector.
Harris: Is Alexandria competing with other localities for PPE from the private sector?
Haering: Well, we are all ordering at the same time. What the city has done is organized itself in what is called a unified command, so that every city department–whether it is the Fire Department or the Department of Community Services–goes through the unified command to order the PPE through the private sector.
Harris: Does Northern Virginia have enough PPE and ventilators ready for when we reach the peak?
Haering: Regarding the ventilators, the hospitals in NOVA–which are all working together and helping each other out in case there is a surge at one hospital–have projected from their models that they are going to be able to handle the surge. Regarding the PPE, there are multiple ways to approach a PPE shortage. The first is that you order more, which we are doing through multiple different vendors. The second thing is to look at the CDC guidance for extended use and for reuse. Extended use means you continue to use the PPE more than once. PPE means a lot of things, but let’s talk about N95 respirators. There is a shortage of respirators, so the healthcare workers continue to wear them after taking care of one patient. Reuse means you go into a patient’s room and you come out, and you’re not doing anything around another patient who is not infectious, and then you put it back on, instead of throwing it away.
Harris: What are the risks of extended use and reuse?
Haering: The risk is not to the patient, but to the healthcare worker. So part of our job is to teach healthcare workers how to safely reuse their masks. The respirator requires training–fit testing is what it is called. Fit testing means we put the respirator on the workers and then we test to make sure that it is working properly and has a proper seal. So healthcare workers are taught how to take respirators off without touching the front of it and then store it properly. The third angle about respirators is decontaminating the respirators. The Food and Drug Administration (FDA) determines that a process or a medical device or a medication is effective, so they have given emergency use authorization for a process that uses hydrogen peroxide, which would basically decontaminate the masks. There is also a number of companies and organizations that have looked at ultraviolet light to decontaminate the respirators.
Harris: You said that Northern Virginia is estimating that we have enough PPE and ventilators to handle this. How much of that can be attributed to social distancing measures?
Haering: It is very hard to say a percentage of how much it has helped. I feel confident that the physical distancing measures that have been put into place by the governor’s order, as well as the city’s measures, have certainly decreased how quickly the numbers would have gone up.
Harris: You said in an interview with the Alexandria Times a couple weeks ago that it is not Alexandria’s job to shut down businesses or get test kits. So what is the city’s role in this?
Haering: The city’s role is to mitigate the impact of the pandemic and the impact of the shutdown on businesses and on residents. The city has worked with businesses and residents to supply them with what the federal government has offered them for small businesses. The city has worked with landlords to ask them to defer the requirement for payment and not to evict people. It doesn’t have the regulatory authority to defer payment requirements but it can make recommendations.
Harris: How well has the federal government lived up to its supposed role in this?
Haering: I think the CDC has been really good at issuing guidance. Quite frankly, I think there has not been a good national strategy. I believe that the White House…has been pretty dismissive of the potential impact from an early stage. The delay of mechanisms put in place to prevent this has put the nation behind the eight ball. The CDC, though, has been exceptionally responsive and proactive in determining the characteristics of the pandemic. Beyond the CDC, there has been a lack of leadership at the national level, but that has not hampered the Virginia response.
Harris: You said earlier we will need mass testing to open up. What else will we need? Will that be enough?
Haering: Some of the things we are looking for is a decrease in the number of cases, and the decrease needs to happen over a 14-day-period. The 14-day-period, by the way, is not arbitrary–it’s the incubation period of the virus. So we want to see a continuous decrease for 14 days. On the healthcare aspect, we need to be able to have a lot of PPE available, as well as massive testing. And on the public health side, we need to have the capacity to do contact tracing on almost all of the positive cases. So if your friend got sick, we would trace down everyone they were in contact with 48 hours before they got sick through the period of the time they did get sick. We call it identifying and isolating. Right now, though, we are in the community mitigation period.
Harris: Do you have any idea of when the identify-and-isolate period will come?
Haering: Well, the governor’s executive order on the shutdown of businesses and the stay-at-home order is extended until June 10. So I do not see that we would be reopening things through May. I, as the health director, will make recommendations to the state, but that is really a decision on the executive level.
Harris: Do you think that we will be able to get back to “normal” before there is a widely available vaccine?
Haering: I think there will be a new type of normal. And that new normal will be on a different kind of test–a blood test that is still in the research phase right now–that tests for antibodies. Hopefully we will be able to have some idea of how many people have had it and are therefore not susceptible to infection or transmission. There is an article in the New York Times today about the way Germany is starting to reopen, but they have a lot of organization and leadership at the national level, but if we can get there then we have a better idea. We can say, “Only 5-10% of the population has had this.” The larger the percentage who test positive for antibodies, the quicker we will get back to normal. I anticipate that if we open up too quickly we will see spikes after this. And that concerns me because the danger of this is really to the elderly–they have a 20% case fatality rate as you get over 65. So it is really incumbent on all of us, who don’t have underlying conditions, to help those people.
Harris: Some places in Asia–Hong Kong, Taiwan, Singapore–are seeing spikes again after the virus showed signs of progress due to incoming travel. Is there any talk of shutting down domestic travel?
Haering: That is not under the local Health Department’s authority. Although, we are telling people coming in from epicenters like New York or New Jersey to quarantine for 14 days. But the thing is, we are telling everyone to stay home right now so there is no big difference in shutting down domestic travel.
Harris: Right. How likely do you think it is that this virus slows down in the summer, mutates and comes back in the fall?
Haering: Well, some viruses have what is called an antigenic shift, which means a shift of how this virus looks to the immune test. We are hoping antibody tests confer immunity, but we won’t know that until later.
Harris: Many people my age are relatively complacent about this virus and have said they want to get the virus just to get it over with. What is your response to that?
Haering: You know, it’s the complacency that has me very concerned because these people don’t recognize that they are contributing to the spread and hitting our vulnerable populations, which include our African American communities, our Hispanic communities, and especially our elderly population. This is one of those situations where my health depends on your health and your health depends on my health.
Harris: Is there any data on how much this has affected African American and Hispanic communities in Alexandria?
Haering: It is available for the state, and the city information will be out tomorrow. It is impacting African American communities in a much more probated (profound) way than the rest of the population. This is why it is so important our invulnerable communities take this seriously as well.